Clinical Care Guidelines
- Clinical Care Guidelines Clinical Care
- Clinical Care Guidelines Preface
- Chapter 1 The Fanconi Anemia DNA Repair Pathway
- Chapter 2 Diagnosis of Fanconi Anemia: Testing and Genetic Counseling
- Chapter 3 Clinical Care of Fanconi Anemia Hematologic Issues
- Chapter 4 Non-HNSCC Solid Tumors in Patients with Fanconi Anemia
- Chapter 5 Head and Neck Cancer in Patients with Fanconi Anemia
- Chapter 6 Oral Health Care for Patients with Fanconi Anemia
- Chapter 7 Gynecologic Care for Female Patients with Fanconi Anemia
- Chapter 8 Dermatologic Issues in Patients with Fanconi Anemia
- Chapter 9 Clinical Care of Fanconi Anemia Gastrointestinal Issues
- Chapter 10 Endocrine Disorders in Patients with Fanconi Anemia
- Chapter 11 Hearing and Ear Issues in Patients with Fanconi Anemia
- Chapter 12 Clinical Care of Hand and Arm Abnormalities in Fanconi Anemia
- Chapter 13 Brief Guide to Clinical Care for Patients with Fanconi Anemia
- Appendix A: Glossary and List of Abbreviations
- List of Contributors
Chapter 12
CLINICAL CARE OF HAND AND ARM ABNORMALITIES IN FANCONI ANEMIA
Introduction
Approximately half of all children with Fanconi anemia (FA) have skeletal abnormalities, most (~70%) of which affect the upper extremities. The most common abnormalities of the upper limbs involve the thumb and radius. Children with these anomalies might have a shortened or absent thumb, radius, or both, due to incomplete growth. Therapy or surgery may be required to maximize the function and appearance of the child’s hands and arms. By the time most FA patients reach adulthood they have completed all necessary hand surgeries in childhood and will not require regular follow-up with their surgeon; how¬ever, occasional evaluation is recommended to check for any developing problems. Unfortunately, many pediatric facilities do not treat adults with pediatric problems. Thus, patients should ask their pediatric hand surgeon to recommend a physician who cares for similar hand and upper extremity abnormalities in adults.
This chapter will describe five common concerns related to the hand and arm in patients with FA:
There are no standardized treatment procedures for congenital hand and arm abnormalities; treatments must be tailored to each child and family. The decision process is multi-factorial and requires participation from the family, physician team, and a physical or occupational therapist.
- Underdeveloped, missing, or duplicated thumb
- Shortened or missing radius
- Shortened, curved forearm
- A hand that develops perpendicularly to the forearm
- Impaired movement in the wrist, fingers, and elbow
INITIAL EVALUATION
Children born with limb abnormalities should be referred to an upper extremity specialist within the first few months of life. This physician should be comfortable with and proficient in the diag-nosis and management of congenital limb anomalies. Ideally, a child with Fanconi anemia (FA) should be referred to a hand and upper limb surgeon who specializes in pediatrics.
Many children with upper limb abnormalities require physical or occupational therapy, which may begin after the initial assessment. A therapist can help to stretch and strengthen the affected limb, fabricate splints, and provide adaptive devices that maximize the patient’s independence. As children get older and begin to perform increasingly complex physical activities, many parents will worry that their child’s impairment is worsening, but in reality, their child’s activities may simply require additional strength and dexterity. A physical or occupational therapist can offer adaptive devices or techniques to help the child accomplish these tasks.
Limb evaluation often occurs before a patient is diagnosed with FA. Because the radius develops at the same time as many organ systems, the physician must evaluate the patient’s entire body. Furthermore, radial deficiency is associated with numerous syndromes, further emphasizing the need for a thorough investigation (Table 1). Many children with VACTERL association have symptoms that are similar to those of children with FA, a diagnostic dilemma that can be solved with the chromosomal breakage test (see Chapter 2). Some patients with VACTERL-H actually have FA, and a combination of radial and renal anomalies is an important clue in this diagnosis [1]. The precise clinical indication for FA testing in children with limb anomalies is still evolving; however, every child with isolated thumb or hand abnormalities or deficiencies with the radius should be tested for FA (see Chapter 2).
Table 1. Syndromes and health conditions associated with radial deficiency.
| Syndrome or Health Condition | Characteristics |
|---|---|
| Holt-Oram Syndrome | Heart defects, particularly defects of the cardiac septa |
| Thrombocytopenia Absent Radius (TAR) Syndrome | – Thrombocytopenia present at birth – May require blood transfusions and can improve over time – Thumbs are present in TAR and may be abnormal in shape |
| VACTERL Association (also discussed in Chapter 2) | – Vertebral abnormalities – Anal atresia – Cardiac abnormalities – Tracheoesophageal fistula – Esophageal atresia – Renal defects – Radial dysplasia Lower limb abnormalities |
| Fanconi anemia | – Aplastic anemia that usually develops in the first decade of life – Thumbs are often absent if radii are absent |
| CHARGE Syndrome | – Coloboma of the eye – Heart defects – Atresia of the nasal choanae – Retardation of growth and/or development – Genital and/or urinary abnormalities – Ear abnormalities and deafness |
Thumb Anomalies
In patients with Fanconi anemia (FA), the thumbs may be underdeveloped or completely absent. The most common types of thumb anomalies that occur in children with FA have been classified into five types of hypoplasia depending on the degree of underdevelopment [2]:
Type I Deficiency
In Type I deficiency, the child’s thumb is slightly smaller than normal, but all of the thumb’s structures (including the bones, muscles, ligaments, tendons, and joints) are present. This mild defi¬ciency may go unrecognized and many individuals are not diagnosed until later in life when everyday activities such as buttoning a shirt or tying shoes become more difficult.
Type II Deficiency
Type II deficiency is more involved and is characterized by a narrowing of the web space between the thumb and index finger, absence of the thenar muscle at the base of the thumb, and instability of the metacarpophalangeal joint in the middle of the thumb (Figure 1A and B).


Figure 1. A two-year-old child with Type II thumb hypoplasia. A) Absent thenar muscles; B) Narrowed thumb-index web space with instability of the metacarpophalangeal joint. Source: Shriners Hospital for Children, Philadelphia Unit.
Type III Deficiency
A child with Type III deficiency possesses the same characteristics as a Type II deficiency, as well as additional skeletal, muscular, and tendinous abnormalities. These abnormalities usually involve tendons that arise within the forearm and travel into the thumb. Type III anoma¬lies are subdivided into Types III-A and III-B depending upon the presence or absence, respectively, of a stable carpometacarpal joint at the base of the thumb.
Distinguishing Between Type III-A and Type III-B Thumb Deficiencies
The clinical differentia¬tion between Type III-A and Type III-B can be difficult. The child’s pattern of thumb usage often helps discriminate between these types. Type III-B thumb deficiencies produce an unstable thumb that will not be incorporated into pinching and grasping motions; rather, the child will learn to pinch and grasp between the index finger and the long digit, and the index finger will tend to rotate out of the palm toward a thumb position. The differentiation is further complicated by the delayed maturation of the bones at the base of the thumb; these bones (the trapezium and trap¬ezoid) do not ossify or become visible on x-ray until 4-6 years of age. Advanced imaging techniques such as magnetic resonance imaging (MRI) can reveal the extent of bone and cartilage development; however, young children require general anesthesia during MRI. Ultrasound imaging shows promise as a tool for defining the trapezium and trap-ezoid anatomy without the need for anesthesia. A thumb metacarpal that tapers to a point at the base of the metacarpal on x-ray also is indicative of an unstable carpometacarpal joint.
Type IV Deficiency
Type IV deficiency, known as a pouce flottant (floating thumb) or residual digit, lacks bones and muscles and is mainly comprised of skin and soft tissue (Figure 2).

Figure 2. A one-year-old child with severe Type IV thumb hypoplasia (also known as a ‘pouce flottant’ or floating thumb). Source: Shriners Hospital for Children, Philadelphia Unit.
Type V Deficiency
Type V deficiency hypoplasia is noted by the complete absence of a thumb (Figure 3).
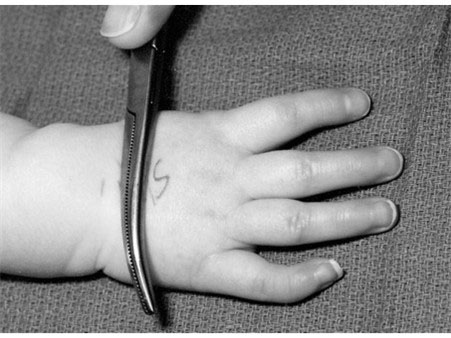
Figure 3. An 18-month-old child with Type V hypoplasia and complete absence of the thumb. Source: Shriners Hospital for Children, Philadelphia Unit.
Thumb classifications can guide treatment recommendations as shown in Table 2 [3-5]. The degree of hypoplasia and deficiency varies among children with FA. As a result, treatment recommendations depend on the severity of the abnormality.
Table 2. Thumb deficiency classification and treatment paradigm.
| Type | Findings | Treatment |
|---|---|---|
| I | Minor generalized hypoplasia | No treatment |
| II | Absence of intrinsic thenar muscles First web space narrowing Ulnar collateral ligament (UCL) insufficiency |
Opponensplasty First-web release UCL reconstruction |
| III | Similar findings as type II AND: Extrinsic muscle and tendon abnormalities Skeletal deficiency Stable carpometacarpal (CMC) joint (sub-Type III-A) Unstable CMC joint (sub-Type III-B) |
Reconstruction (for sub-Type III-A) Pollicization (for sub-Type III-B) |
| IV | “Pouce flottant” or floating thumb | Pollicization |
| V | Absent thumb | Pollicization |
TREATMENTS FOR HYPOPLASTIC, FLOATING, AND ABSENT THUMBS
A thumb that is slightly smaller than normal (Type I) does not require surgical reconstruction. Type II and III-A thumbs can be reconstructed; however, multiple elements need to be addressed during surgery to maximize the thumb’s function (Figure 4A thru C):
- Tightness in the web space can be released using skin flaps to increase the space between the thumb and index finger (Figure 4A).
- Thenar muscle deficiency can be treated by transferring tendon and/or muscle from the ring or long finger to the thumb. Tendon transfer improves the active motion and function of the thumb and has a negligible effect on the donor finger (Figure 4B).
- Metacarpophalangeal joint instability can be improved by reconstructing the ligaments using tendon grafts to the ulnar and/or radial collateral liga¬ments at the base of the thumb (Figure 4C). In cases with severe instability, fusion of the joint may be the best option to provide a stable thumb for firm grasp.
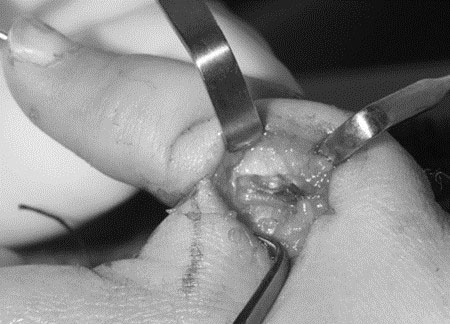
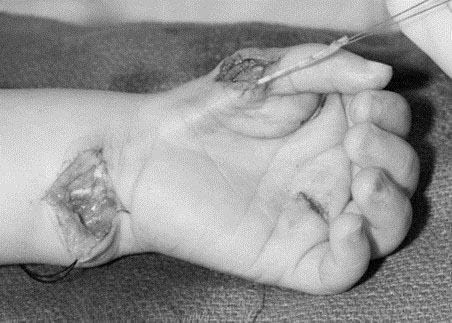
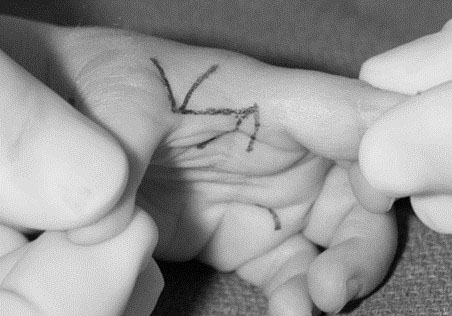
Figure 4. Thumb reconstruction for Types II and III-A requires the surgeon to address all deficient elements. A) Z-plasty of the narrowed thumb-index web space; B) Tendon transfer to overcome the deficient thenar muscles; C) Ligament reconstruction to stabilize the metacarpophalangeal joint instability. Source: Shriners Hospital for Children, Philadelphia Unit.
The main distinction between a thumb that can be surgically reconstructed and a thumb that requires amputation is the presence or absence of a stable base (e.g., a carpometacar¬pal joint). A thumb without a stable carpometacarpal joint (Types III-B, IV, and V) cannot be reconstructed and should be removed. Clinical examination and x-ray will show marked deficiencies (Figures 5 and 6).
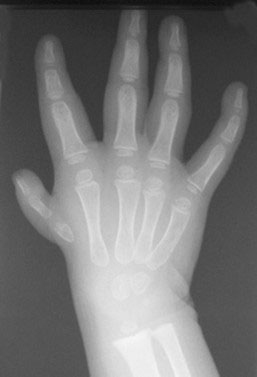
Figure 5. An X-ray of a two-year-old child reveals a thumb metacarpal that tapers to a point, indicative of an unstable carpometacarpal joint. Source: Shriners Hospital for Children, Philadelphia Unit.

Figure 6. A five-year-old child with bilateral thumb hypoplasia. The right index-long web space has widened and the index has rotated out of the palm. Source: Shriners Hospital for Children, Philadelphia Unit.
In addition, Type III-B and IV thumbs are not functional, and the child will not incorporate his/her thumb into pinch or grasp. The decision to remove a hypoplastic thumb without a stable base often is a difficult process for parents and care¬givers. Discussions with the surgeon and conversations with families who have made similar decisions often are helpful to parents tasked with making this decision for their child.
Following removal of a hypoplastic thumb, creation of an opposable thumb is critical for grasp and object manipulation. The preferred procedure is pollicization, which involves moving the index finger and its nerves, arteries, tendons, and muscles to the thumb position. Pollicization requires meticulous surgical technique because the index finger must be shortened, rotated, and reconstructed with the index muscles to give the appearance and function of a thumb (Figure 7). The surgeon should be experi¬enced with this procedure. This procedure is generally performed when the child is between 6-24 months of age, depending on the health status of the child, the degree of forearm deficiency, and the surgeon’s preference [2, 3]. The general medical health of a child with FA also should be taken into consideration prior to surgery, especially if the child’s blood counts are decreasing over time. Surgery can be safely performed in patients who have platelet counts greater than 80,000. In reality, parents should not feel pressured to make an immediate decision about surgery for their child. Some children undergo successful surgery during adolescence, though acceptance of a change in the appearance and composition of their hand can be more difficult.
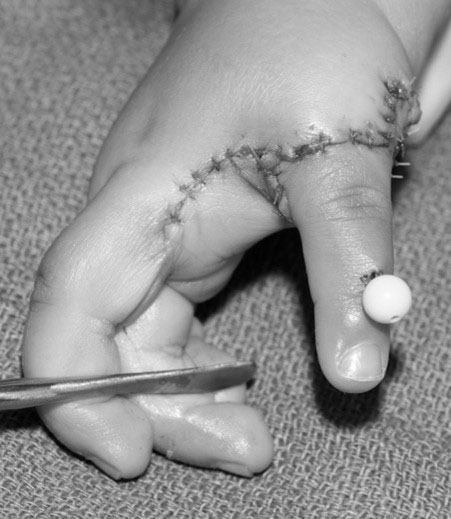
Figure 7. Pollicization of the index finger requires careful surgical technique to give the appearance and function of a thumb. Source: Shriners Hospital for Children, Philadelphia Unit.
The outcome of pollicization is directly related to the status of the index finger prior to surgery. A mobile index finger can provide stability for grasp and mobility for fine pinch, whereas a stiff index finger will provide a stable thumb for coarse grasping, but fine pinching will be unlikely (Figure 8). Good results shortly after pollicization have been shown to persist into adulthood [6, 7].


Figure 8. A two-year-old’s status post-pollicization of a mobile left index finger. A) Thumb used for grasping large objects; B) Mobile thumb incorporated into fine pinch. Source: Shriners Hospital for Children, Philadelphia Unit.
OTHER THUMB ANOMALIES
Although hypoplasia is the most common thumb anomaly in children with FA, other abnormalities have been reported. For example, the thumb can possess an extra bone (an anomaly referred to as a triphalangeal thumb) or can be duplicated (a condition called pre-axial polydactyly). The exact prevalence of these rare anomalies is unknown.
Triphalangeal thumb
A triphalangeal thumb has an extra phalanx that can vary in size and shape (Figure 9). The alignment and length of this type of thumb must be monitored during growth. An extra phalanx that is small and normally shaped can be treated without surgery; however, a small wedge-shaped phalanx may cause the thumb to curve as it grows, and treatment is rec¬ommended. A small wedge-shaped bone can be surgically removed, and the ligaments of the remaining bones can be reconstructed to form a functional joint. A large wedge-shaped phalanx that causes the thumb to curve and become excessively long should not be removed because joint instability is common following surgery. A better option involves removing only the wedge-shaped portion of the abnormal phalanx and fusing the remainder to an adjacent thumb bone. This pro¬cedure realigns the thumb, shortens the elongated thumb, and eliminates the extra joint.

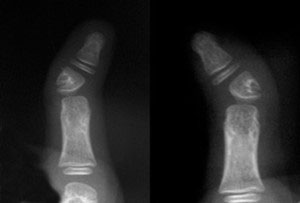
Figure 9. Eight-year-old child with triphalangeal thumbs. A) Clinical appearance with mild angulation; B) X-rays show an extra phalanx that is triangular in shape causing the angulation. Source: Shriners Hospital for Children, Philadelphia Unit.
Pre-Axial Polydactyly
Pre-axial polydactyly, or duplication of the thumb, results in a hand that has more than one thumb. The thumbs may be partial and appear fused together, or they may be complete and separate from each other. Thumb duplications have been classified into various types depending on the degree of skeletal replication (Table 3) [8, 9]. Treatment requires salvaging portions of each duplicated structure, including bones, nails, tendons, ligaments, joints, nerves, and blood vessels, to construct a properly aligned and functional thumb (Figure 10) [10]. This procedure is not always straightforward and requires careful intra-operative decision making. The soft tissues from the amputated thumb, including the skin, nail, ligaments, and muscle, should be used to augment the retained thumb. The articular surface of the joint may require realignment via osteotomy and modification via cartilage shaving to optimize thumb function. Irrespective of treatment, the recon¬structed thumb may be smaller compared to a normal thumb and usually will lack some movement.
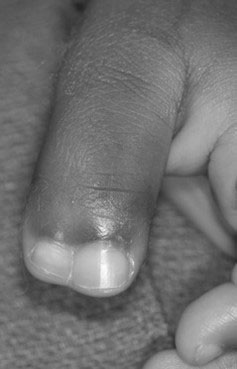
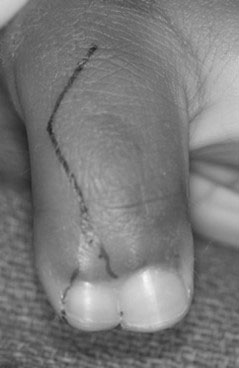
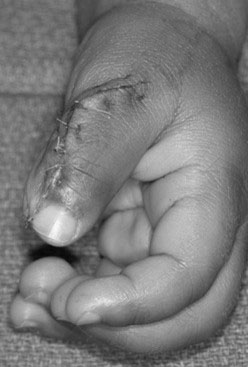
Figure 10. A one-year-old child with a duplicated left thumb. A) Clinical presentation; B) Skin incision designed to incorporate parts of the deleted component; C) Surgical reconstruction using the soft tissues from the deleted thumb to augment the size and girth of the retained thumb. Source: Shriners Hospital for Children, Philadelphia Unit.
Table 3. Classification of duplicated thumbs.
| Type | Duplicated Elements |
|---|---|
| I | Bifid distal phalanx (a partial duplication of the bone at the tip of the thumb) |
| II | Duplicated distal phalanx (a complete duplication of the bone at the tip of the thumb) |
| III | Bifid proximal phalanx (a partial duplication of the bone in the middle of the thumb) |
| IV | Duplicated proximal phalanx* (a complete duplication of the bone in the middle of the thumb) |
| V | Bifid metacarpal phalanx (a partial duplication of the bone that connects the thumb to the wrist) |
| VI | Duplicated metacarpal phalanx (a complete duplication of the bone that connects the thumb to the wrist |
| VII | Triphalangeal component (a thumb duplication with one or both of the thumbs having an extra phalanx or bone) |
*Most common type of duplicated thumb. Modified from reference [9].
Radial Deficiency
Radial deficiency is a skeletal condition in which the radius develops abnormally. The radius can be slightly smaller than average, considerably smaller, or altogether absent. The severity of radial deficiency is variable and can be determined through x-rays and clinical examination. Radial deficiency is classified as follows [11, 12]:
- Type 0 and 1 deficiencies. These are the mildest forms and are charac¬terized by little or no shortening of the radius and negligible curvature in the ulna. The hand may be tilted slightly inward toward the thumb side of the arm, a condition known as a radial deviation of the wrist, and substantial thumb hypoplasia may be present that requires treatment.
- Type 2 deficiency. This deficiency is characterized by a miniature radius that has abnor-malities in the growth plate (the region of the bone responsible for lengthening the bone) and a moderate radial deviation of the wrist.
- Type 3 deficiency. This involves a partial substantial absence of the radius—most commonly affecting the end of the bone that is closest to the wrist—and a severe radial deviation of the wrist.
- Type 4 deficiency. In the most common type of radial deficiency, characterized by a complete absence of the radius, the hand tends to develop perpendicularly to the forearm (Figure 11A and B). In chil¬dren with FA, a complete absence of the radius typically occurs in conjunction with an absent thumb.
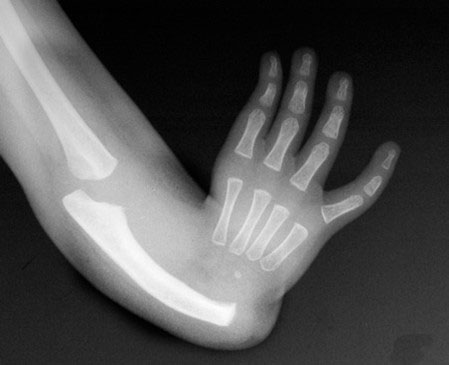
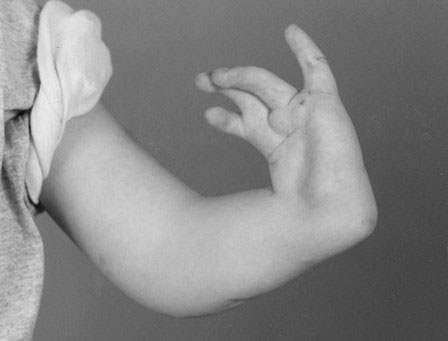
Figure 11. A two-year-old child with complete absence of the radius (Type 4). A) X-ray reveals complete absence of the radius; B) Hand with a perpendicular relation¬ship with the forearm. Source: Shriners Hospital for Children, Philadelphia Unit.
The maturation of the radius takes more time than usual in patients with radial deficiency; therefore, the differentiation between total and partial absence (Types 3 and 4) cannot be determined until the child is approximately three years of age. The different types of radial deficiencies have been combined into a classification scheme that includes the other upper limb abnormalities that are associated with radial deficiency, including thumb, carpal, and forearm abnormalities (Table 4).
Table 4. Classification of radial longitudinal deficiency.
| Type | Thumb | Carpus | Distal radius | Proximal radius |
|---|---|---|---|---|
| N | Hypoplastic or absent | Normal | Normal | Normal |
| 0 | Hypoplastic or absent | Absence, hypoplasia, or coalition | Normal | Normal, radioulnar synostosis, or congenital dislocation of the radial head |
| 1 | Hypoplastic or absent | Absence, hypoplasia, or coalition | > 2 mm shorter than ulna | Normal, radioulnar synostosis, or congenital dislocation of the radial head |
| 2 | Hypoplastic or absent | Absence, hypoplasia, or coalition | Hypoplasia | Hypoplasia |
| 3 | Hypoplastic or absent | Absence, hypoplasia, or coalition | Physis absent | Variable hypoplasia |
| 4 | Hypoplastic or absent | Absence, hypoplasia, or coalition | Absent | Absent |
Modified from references [11] and [12].
Functional Consequences of Radial Deficiency
The outcome of radial deficiency depends on the severity of the abnormality. In a patient with a Type 4 deficiency, the humerus may be shorter than expected and the elbow may not bend properly. Furthermore, the forearm will always be shortened because the ulna is approxi¬mately 60% of the normal length at birth and remains short even after the skeleton has completely grown and matured [13]. The ulna also will be thickened and often curved toward the absent radius. In cases of partial or complete absence of the radius, the forearm will not be able to rotate, although some rotation may occur through the wrist or carpal bones. The wrist may be shifted a vari¬able amount towards the deficient radius, a condition known as a radial deviation. The carpal bones will be delayed in their growth, and the scaphoid and trapezium often are absent or hypoplastic. The index and middle fingers can be stiff and slender and may have limited motion, whereas the ring and little fingers are less affected and often have better motion.
The radial artery and nerve are often absent, although the ulnar nerve and artery are normal [13]. An enlarged median nerve substitutes for the absent radial nerve and communicates with its dorsal nerve branch, which is positioned in the fold between the wrist and forearm, to provide sensation to the thumb side of the hand. It is critical that surgeons are aware of the location of the dorsal branch when operating along the thumb side of the wrist.
Radial Deficiency Treatment Considerations
The fundamental goals of treatment are to correct the radial deviation of the wrist to balance the wrist and forearm while maintaining range of motion for the wrist and fingers. Treatment also should strive to promote growth or lengthening of the forearm and improve the overall function of the arm. A slightly shortened radius (Type 0 and 1 deficiencies) requires repeated stretching and occasionally requires a tendon transfer to balance the wrist. These treatments are rela¬tively straightforward. Partial or complete absence of the radius is more common (Types 2, 3, and 4) and is entirely more difficult to treat because the wrist has shifted toward the thumb side of the arm, shortening an already undersized forearm, placing the forearm flexor and extensor ten¬dons at an awkward angle, and producing functional deficits. Children who have unilateral radial deficiency may be able to compensate for any functional deficits using their unaffected limb and, therefore, have a lower overall degree of functional impairment compared to children who have bilateral radial deficiency. Finger and thumb abnormali¬ties, if present, also require consideration during the formulation of a treatment plan, as stiff fingers and a deficient thumb will further hamper abilities to pinch and grasp.
Radial Deficiency Nonsurgical Treatments
The initial treatment for an absent radius should begin shortly after birth and consists of stretching the soft tissues, including the tendons, ligaments, skin, and muscles. This treatment is typically performed by both a physical or occupational therapist and the caregiver. The therapist should be experienced in pediatric clinical interventions for the hand. Stretching should be performed at every diaper change and is an important part of the overall treatment plan. A splint can help to keep the hand in a straight alignment and prevent the hand from developing perpendicularly to the forearm; however, fabrication of a splint is difficult in a new¬born with a shortened forearm because the splints tend to fall off the arm. Therefore, this treatment is usually postponed until the forearm is long enough to accommodate a splint. On occasion, the hand will develop in a perpendicular position despite stretching and splinting treatments.
Radial Deficiency Surgical Treatment
Surgical treatment for Types 2, 3, and 4 deficiencies involves moving and centering the wrist over the end of the ulna, which is the only substantial bone remaining within the forearm. This procedure is known as “centralization” or “radializa¬tion” depending on the exact position in which the wrist is placed, and remains the standard treatment for realigning the wrist [14, 15]. Centraliza¬tion involves releasing and reorganizing the tight muscles and tendons of the wrist and positioning the hand over the end of the ulna (Figure 12).
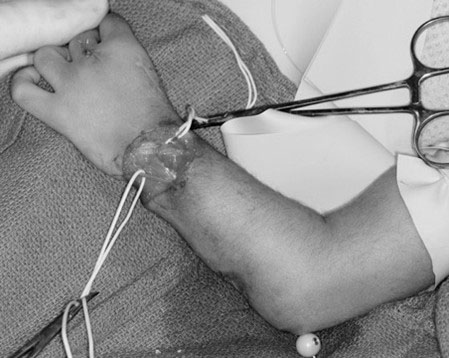
Figure 12. Surgical centralization requires placing the wrist on top of the ulna to realign the carpus onto the distal ulna. Source: Shriners Hospital for Children, Philadelphia Unit.
One end of a functioning tendon is then shifted from its original attachment site to the wrist to rebalance the forces acting on the wrist, a procedure known as tendon transfer. If the ulna has curved to an angle of 30 degrees or more, then it must be straightened via a procedure called wedge osteotomy at the time of surgery. Once the surgery is complete, the wrist is held in position by a stout wire (Figure 13), which can be removed 8-12 weeks after surgery, although some surgeons prefer to leave the wire in place for as long as possible. Once the wire has been removed, a splint should be used for at least 4-6 weeks. The splint can be removed for physical therapy exercises, but most surgeons recommend that the splint be worn during sleep until the child has stopped growing.
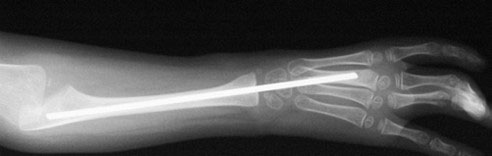
Figure 13. Centralization is maintained by placement of a stout wire across the wrist. Source: Shriners Hospital for Children, Philadelphia Unit.
Centralization typically is performed when the child reaches approximately one year of age. The initial correction is often impressive; however, the results are unpredictable and, unfortu¬nately, recurrence and complications are common. Furthermore, not all children are candidates for centralization. The caregiver and surgeon must remember that “function trumps form,” and many children function quite well despite having a deviated wrist. Such children typically have a mobile and dexterous little finger along with a stiff index finger, and are best able to pinch and grasp using their palm and the fingers on the outside edge of the hand, known as an ulnar grasp pattern. In these children, straightening the child’s wrist would move the outside edge and fingers downward and prevent the child from approaching objects with this side of the hand. Therefore, straightening may be detrimental to the child’s overall function and independence.
In an effort to maintain motion and obtain partial correction of the radial deviation, a surgeon may find it useful to use a soft tissue release and skin flap to avoid entering the joint and jeopardizing growth and motion [16]. High satisfaction rates and functionality scores have been reported even though the forearm remained angulated after surgery. This technique involves a bilobed flap to transpose the excess ulnar-sided soft tissue to the radial side of the wrist (Figure 14). All underlying tight fascial bands are released and wrist flexors with a purely radial deviating force are cut or transferred. The ulnocarpal joint is not opened and a formal centralization is not performed. Concomitant ulnar osteotomy is performed if angulation exceeds 30 degrees.
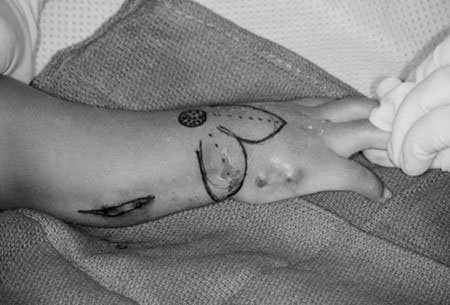
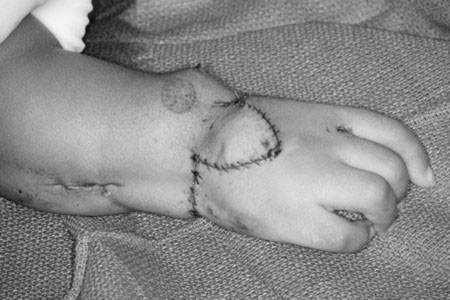
Figure 14. Soft tissue release and skin flap procedure. A) Design of bilobed flap to transpose dorsal skin to the radial side of the wrist and the excessive ulnar-sided skin to dorsum of the wrist for added dermodesis; B) Flap inset and closure after transposition of dorsal and ulnar flaps. Source: Shriners Hospital for Children, Philadelphia Unit.
Contraindications for Surgery
Mild deformities with adequate support for the hand (Type 0 or 1) do not require surgery. Surgery also is not advised for children with limited ability to bend the elbow. In these children, the radial devia¬tion of the wrist enables the hand to reach the mouth and straightening the wrist would impair important tasks such as eating and reaching the face.
Alternative Treatments for Recurrent Radial Deviation
In severe cases, the radial deviation can¬not be straightened and alternative measures are necessary. Surgical options include removing a portion of the wrist bones via a procedure called carpectomy, shaving some of the bone off the wrist end of the ulna, or applying a device called an exter¬nal fixator prior to centralization. An external fixator stretches the soft tissues (including the tendons, ligaments, skin, and muscles) prior to centralization and facilitates correction of the radial deviation [17-19]. The fixator may be unilateral with pins or ringed multiplanar with wires (Figure 15).
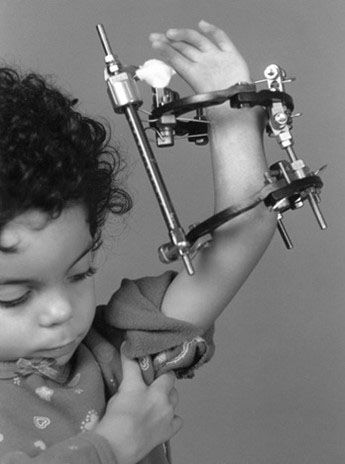
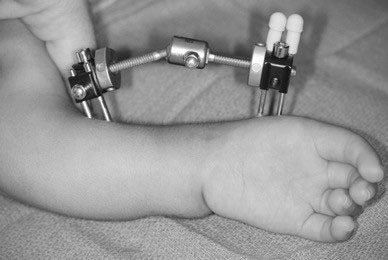
Figure 15. Radial deficiency with rigid deformity is treated with preliminary soft tissue distraction. A) Uniplanar device along the radial side of the forearm; B) Multiplanar device for additional control of hand and forearm. Source: Shriners Hospital for Children, Philadelphia Unit.
Numerous other technical modifications have been proposed to maintain alignment of the wrist position. These include overcorrection of the radiation deviation, tendon transfers to correct the alignment, prolonged wire fixation following centralization (leaving the wire in place for longer than the typical 8-12 weeks), and microvascular free toe transfer. Overcorrection of the radial deviation requires the patient’s hand to be positioned slightly off-center into ulnar deviation to help prevent recurrence of the radial deviation. Microvascular free toe transfer involves transplanting one of the second toes (without its skin but with its arteries and veins intact) to the thumb side of the wrist to provide additional support (Figure 16). A study of the outcomes of this procedure during an 8-year period revealed that patients tended to have improved wrist motion and limited recurrence [20]. This is a technically demanding operation, however, and complications are common.

Figure 16. Diagram of free toe transfer to support the radial side of the wrist. The toe proximal phalanx is fused to the base of the second metacarpal and the proximal metatarsal affixed to the side of the distal ulna. Reprinted with permission [21].
Treatment Outcomes for Radial Deviation Correction
Unfortunately, no single treatment method consistently and permanently cor¬rects the radial deviation, balances the wrist, and allows continued growth of the forearm [14, 15]. Recurrence can prove frustrating to the child, parent, and surgeon (Figure 17). Maintaining the wrist on the end of the ulna without sacrificing wrist mobility or stunting forearm growth remains a daunting task. Many factors contribute to recurrence, including the inability to obtain complete correction at surgery, inad¬equate release of the tightness in the soft tissues, and failure to balance the forces acting on the wrist. Prolonged wire fixation and use of a splint may help minimize recurrence. In some children, there is a natural tendency for the shortened forearm and hand to deviate in a radial direction for hand-to-mouth use. Fortunately, recurrence is not always associated with a loss of function. Although patients with severe radial deviation may have limitations in their range of motion and strength, long-term studies have found that they function independently and participate in a high number of activities that is comparable to children with less severe deformities [22-25].

Figure 17. An 11-year-old child with recurrent radial deviation following centralization as an infant. Source: Shriners Hospital for Children, Philadelphia Unit.
A 2017 study examined the long-term outcome of surgical or nonsurgical treatment of children with radial deficiency [26]. Non-surgical patients had the most radial deviation and forearm angulation. Soft tissue release and bilobed flap lessened the radial deviation without causing physeal arrest and maintaining good wrist motion. External fixation and subsequent centralization or radialization achieved the best angular correction but resulted in the decreased wrist motion and shortened the ulnar length. Microvascular toe transfer that connected the distal ulna to the carpus resulted in the best motion while maintaining good ulnar length.
The management of recurrent deformity must be indi¬vidualized to each patient and the specifics of his/her defor¬mity. Similarly, the indication for fore¬arm lengthening to overcome the inherent problem of a shortened forearm have yet to be delineated. Lengthening surgery is offered to patients and families interested in correcting the deformity and willing to comply with a long and arduous recovery. The procedure, called distraction osteogenesis, involves inducing new bone growth, typically by pulling on the bone in a controlled manner using an external fixator (Figure 18). Lengthening is a sophisticated form of treatment that introduces addi¬tional complications such as infection at the insertion sites of the external fixator, fracture of the regenerated bone, and finger stiffness. These complications must be discussed prior to surgery. Forearm lengthening is laborious and may require the device to remain in place for extended periods of time, sometimes up to a year. In general, children with unilateral forearm shortening tend to be bothered by the asymmetry between the forearms and request lengthening more often than children with bilaterally shortened forearms, who have symmetry between the arms.
Ultimately, fusion of the joint between the wrist and ulna may be con¬templated in certain instances to keep the wrist straight [27]. Wrist fusion results in a permanently stiff, straight wrist. Careful assessment of hand usage and compensa¬tory motion is mandatory prior to this procedure. A functional evaluation by a physical therapist is a valuable preop¬erative tool. Painstaking measures should be taken to ensure that wrist fusion does not lead to loss of function.

Figure 18. Bilateral forearm lengthening using an external fixator. Source: Shriners Hospital for Children, Philadelphia Unit.
Summary
Upper extremity skeletal abnormalities such as thumb and radial deficiencies are common in patients with Fanconi anemia (FA). Evaluation of skeletal abnormalities typically precedes diagnosis of FA and can be used as criteria for further evaluation during diagnosis of the disease. Mild to severe hypoplastic thumb deficiencies may require surgical intervention depending on the severity of the anomaly and other patient-specific factors. Radial deficiencies are variable and characterized by a radius that can be smaller than average, or altogether absent. The treatment for radial abnormalities ranges from soft tissue stretching for mild cases to surgical intervention for more severe cases. The goals of treatment are to correct the radial deviation while promoting forearm lengthening and improving the overall function of the arm. Treatment for radial abnormalities, regardless of the modality used, may not be permanent and recurrence is possible.
The Fanconi Anemia Research Fund recognizes the following author contributions to the 5th edition:
Scott H. Kozin, MD*
Roger Cornwall, MD
Ann Van Heest, MD
*Chapter Committee Chair
- Previous Chapter: Chapter 11
- Next Chapter: Chapter 13
References
- Alter, B.P. and P.S. Rosenberg, VACTERL-H association and Fanconi anemia. Mol Syndromol, 2013. 4(1-2): p. 87-93.
- Lister, G., Reconstruction of the hypoplastic thumb. Clin Orthop Relat Res, 1985(195): p. 52-65.
- Kozin, S.H., et al., Index finger pollicization for congenital aplasia or hypoplasia of the thumb. J Hand Surg Am, 1992. 17(5): p. 880-4.
- Manske, P.R., H.R. McCarroll, Jr., and M. James, Type III-A hypoplastic thumb. J Hand Surg Am, 1995. 20(2): p. 246-53.
- Graham, T.J. and D.S. Louis, A comprehensive approach to surgical management of the type IIIA hypoplastic thumb. J Hand Surg Am, 1998. 23(1): p. 3-13.
- Clark, D.I., J. Chell, and T.R. Davis, Pollicisation of the index finger. A 27-year follow-up study. J Bone Joint Surg Br, 1998. 80(4): p. 631-5.
- Kozin, S.H., Pollicization: the concept, technical details, and outcome. Clin Orthop Surg, 2012. 4(1): p. 18-35.
- Cohen, M.S., Thumb duplication. Hand Clin, 1998. 14(1): p. 17-27.
- Wassel, H.D., The results of surgery for polydactyly of the thumb. A review. Clin Orthop Relat Res, 1969. 64: p. 175-93.
- Dobyns, J.H., P.R. Lipscomb, and W.P. Cooney, Management of thumb duplication. Clin Orthop Relat Res, 1985. 195: p. 26-44.
- James, M.A., H.R. McCarroll, Jr., and P.R. Manske, The spectrum of radial longitudinal deficiency: a modified classification. J Hand Surg Am, 1999. 24(6): p. 1145-55.
- Bayne, L.G. and M.S. Klug, Long-term review of the surgical treatment of radial deficiencies. J Hand Surg Am, 1987. 12(2): p. 169-79.
- Heikel, H.V., Aplasia and hypoplasia of the radius: studies on 64 cases and on epiphyseal transplantation in rabbits with the imitated defect. Acta Orthop Scand Suppl, 1959. 39: p. 1-155.
- Bora, F.W., Jr., et al., Radial club-hand deformity. Long-term follow-up. J Bone Joint Surg Am, 1981. 63(5): p. 741-5.
- Damore, E., et al., The recurrence of deformity after surgical centralization for radial clubhand. J Hand Surg Am, 2000. 25(4): p. 745-51.
- Vuillermin, C., et al., Soft tissue release and bilobed flap for severe radial longitudinal deficiency. J Hand Surg Am, 2015. 40(5): p. 894-9.
- Goldfarb, C.A., et al., Soft-tissue distraction with a ring external fixator before centralization for radial longitudinal deficiency. J Hand Surg Am, 2006. 31(6): p. 952-9.
- Nanchahal, J. and M.A. Tonkin, Pre-operative distraction lengthening for radial longitudinal deficiency. J Hand Surg Br, 1996. 21(1): p. 103-7.
- Taghinia, A.H., A.A. Al-Sheikh, and J. Upton, Preoperative soft-tissue distraction for radial longitudinal deficiency: an analysis of indications and outcomes. Plast Reconstr Surg, 2007. 120(5): p. 1305-12; discussion 1313-4.
- Vilkki, S.K., Distraction and microvascular epiphysis transfer for radial club hand. J Hand Surg Br, 1998. 23(4): p. 445-52.
- Kozin, S.H., Congenital Anomalies. Hand Surgery Update, ed. T.E. Trumble and J.E. Budoff. 2007: American Society for Surgery of the Hand.
- Goldfarb, C.A., et al., Functional outcome after centralization for radius dysplasia. J Hand Surg Am, 2002. 27(1): p. 118-24.
- Holtslag, I., et al., Long-term functional outcome of patients with longitudinal radial deficiency: cross-sectional evaluation of function, activity and participation. Disabil Rehabil, 2013. 35(16): p. 1401-7.
- Dana, C., et al., Recurrence of radial bowing after soft tissue distraction and subsequent radialization for radial longitudinal deficiency. J Hand Surg Am, 2012. 37(10): p. 2082-7.
- Kotwal, P.P., M.K. Varshney, and A. Soral, Comparison of surgical treatment and nonoperative management for radial longitudinal deficiency. J Hand Surg Eur Vol, 2012. 37(2): p. 161-9.
- Murphy, G.R.F., et al., Correction of "wrist" deformity in radial dysplasia: A systematic review and meta-analysis. J Bone Joint Surg Am, 2017. 99(24): p. 2120-26.
- Pike, J.M., et al., Ulnocarpal epiphyseal arthrodesis for recurrent deformity after centralization for radial longitudinal deficiency. J Hand Surg Am, 2010. 35(11): p. 1755-61.
- Bradbury, E., Psychological issues for children and their parents., in Congenital Malformations of the Hand and Forearm, D. Buck-Gramcko, Editor. 1998, Churchill Livingstone: London. p. 48-56.

